Nuchal Translucency (NT) Scan: What the Results Mean
Throughout pregnancy, you and your baby will have to go through countless checkups and tests. One relatively early—albeit optional—example is the nuchal translucency (NT) scan.
- What is a nuchal translucency scan?
- What’s the difference between nuchal translucency scans and non-invasive prenatal testing?
- What to expect from a nuchal translucency scan
- How to interpret your nuchal translucency scan results
- What if your nuchal translucency scan spots a potential issue?
- Do you have to get a nuchal translucency scan?
- Final thoughts
Many expecting parents get a little anxious about the nuchal translucency (NT) screening. What exactly does it reveal about your developing baby, and what does it mean if she receives an “abnormal” result?
We’ll demystify the NT scan and put any worries that might be sending your mind into a tailspin of what-ifs before your appointment to rest.
What is a nuchal translucency scan?
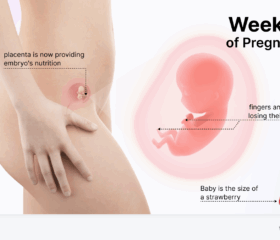
A nuchal translucency (NT) scan is an optional ultrasound you can have when you’re between 11 weeks pregnant and 14 weeks pregnant. 1
Doctors often combine it with blood work (part of your first trimester screening) to help gauge your baby’s chances of having genetic or chromosomal abnormalities. 2
What does the scan check for?
The NT scan is a screening test, not a diagnostic one. Its purpose is to help determine the risk of these conditions, not to confirm them.
The target conditions include Down syndrome (trisomy 21, or having three copies instead of two copies of chromosome 21), Edwards syndrome (trisomy 18), Patau syndrome (trisomy 13), congenital heart defects, and skeletal issues. 3
During the scan, your sonographer will measure the clear space at the back of your baby’s neck. This is the nuchal translucency. All babies have this, but those with certain chromosomal abnormalities tend to have more fluid accumulation in this area during the first trimester.
Time is of the essence with NT screenings. The fluid behind your baby’s neck will get reabsorbed by her body after 14 weeks. 4
What’s the difference between nuchal translucency scans and non-invasive prenatal testing?
The NT scan and non-invasive prenatal testing (NIPT) work hand in hand. The latter is a blood test, but you shouldn’t confuse it with the blood work that typically accompanies an NT scan as part of the so-called “combined first trimester screening.” NIPT analyzes the fetal DNA in your blood for chromosomal abnormalities.
While the NT scan and NIPT both check for common conditions, they have distinct differences and advantages.
NIPT, for example, won’t pick up on potential heart defects like an NT scan will. On the other hand, NIPT can determine your baby’s sex, unlike an NT scan.
You can receive NIPT at any point after 9 weeks into your pregnancy, but will typically test when you’re between 11 and 14 weeks pregnant if you want it to complement the more time-sensitive NT scan. 5
Why are both scans important?
A standalone NT scan could return a false positive. With its 98%–99% detection rate for Down syndrome, Edwards Syndrome, and Patau Syndrome, NIPT acts as a second sanity check (although if either test is abnormal, the recommendation is for diagnostic testing and not just another screening test). 6 7
If you get the NT scan and NIPT in your first trimester, you and your pregnancy team can get valuable details early and use them to inform your future decision-making.
Again, to reiterate, the name of the game here is risk assessment, not diagnosis. If the risk is there, you can opt for further diagnostic testing.
What to expect from a nuchal translucency scan
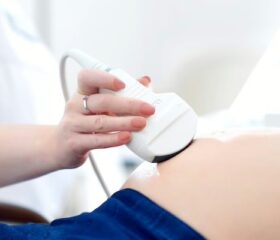
A trained and certified ultrasound technician, maternal-fetal medicine specialist, or clinician will perform the NT ultrasound either transvaginally or abdominally. 8
With either ultrasound, the sonographer will confirm your baby’s gestational age by measuring him from crown to rump. Your tech will then carefully measure the thickness of his nuchal translucency.
Some technicians will also check to see if your baby’s fetal nasal bone is present during the NT scan. This structure’s absence might signify an increased likelihood of chromosomal abnormalities. 9
Abdominal ultrasounds
If you get an abdominal ultrasound, you may get instructions to come in with a full bladder (for better visualization). Your tech will put gel on your abdomen and move a probe over your skin to get a visual of your baby. Expect some light pressure.
Transvaginal ultrasounds
If you get a transvaginal ultrasound, you’ll enter the office with an empty bladder. Your technician will insert a probe into your vagina to pick up a clearer image of the baby. There will be some pressure in your pelvic area, but things shouldn’t get painful.
How to interpret your nuchal translucency scan results
After the NT scan and blood work, you’ll get your results, which will include the NT measurement in millimeters, your baby’s length (which corresponds to his gestational age), your own age, and chemical measurements in your blood.
This result will come with a “risk ratio.” For example, if your ratio is 1 in 100, that means that for every 100 women with this result, a single baby will have the target condition, and 99 won’t. That would be a fairly high risk ratio. A result of 1 in 1,000 indicates a much lower risk. 10
What’s a normal vs. abnormal NT measurement?
Keep in mind that a “normal” result doesn’t guarantee your baby has normal chromosomes. It merely suggests that a problem is unlikely. Conversely, “abnormal” doesn’t necessarily mean there will be a problem.
The normal or abnormal distinction changes based on absolute NT measurement and gestational age, with a majority of international guidelines using the “95th percentile” as the normal NT cutoff.
Experts view an NT measurement below this calculation as “normal” (i.e., over 95 out of 100 screen results have a lower chance of developing chromosomal abnormalities). If a combined NT measurement and blood test presents a risk of higher than 1 in 150, expect your doctor to recommend additional testing. 11
Are false negative or false positive results possible?
While the NT scan is generally accurate, screenings aren’t perfect, and errors can occur.
NT scans miss Down syndrome in about 30–36 out of 100 fetuses. 12 Conversely, you could also get a false positive result, where your NT screening suggests that your baby has an increased risk of a congenital issue even if there’s nothing wrong. 12
Again, because the NT scan isn’t perfectly reliable—no medical tests are!—it can be paired with NIPT and other prenatal screenings.
What if your nuchal translucency scan spots a potential issue?
Here’s where diagnostic testing takes over to confirm or rule out the risk assessment results. Your doctor may suggest you get chorionic villus sampling (CVS), where they analyze placental tissue between week 10 and week 13 of your pregnancy. 13
They also might recommend amniocentesis, where they’ll take a sample of your amniotic fluid, although this can only happen after week 15. 14
They could also perform a fetal echocardiogram when you’re around 20 weeks pregnant, which involves a detailed ultrasound of your baby’s heart to look for structural defects. 15
Consider speaking with a genetic counselor
While most cases of Down syndrome aren’t inherited, some forms of it (e.g., translocation Down syndrome) can be passed to a baby from an unaffected parent. Your doctor might be able to direct you to a genetic counselor who can look over your results and your family history with you and discuss your options if they spot any possible issues.
Do you have to get a nuchal translucency scan?
The American College of Obstetricians and Gynecologists (ACOG) recommends offering prenatal genetic screening for all pregnant women, regardless of age and risk factors. This includes an NT ultrasound. 16
However, some women prefer to go in blind and skip any prenatal testing. Others view a heads-up about potential issues as empowering, especially if it means giving them extra time to prepare for the possibility of a child with special needs.
This decision is yours to make. Think about your values, your comfort with potentially concerning news, your willingness to undergo further testing, and practical considerations like your insurance coverage. (Generally, insurance covers NT scans, but out-of-pocket costs may vary depending on your plan and the testing center.)
Final thoughts
The thought of getting a nuchal translucency scan may make you lose a little sleep. It’s important to remember that it’s just a screening, and the odds are high that things will work out in your little one’s favor.
At this point, all you can do is armor up with as much knowledge as possible so you can decide what’s best for you and your little passenger, whatever you learn.
Article Sources
- MedlinePlus. "Nuchal translucency test" Retrieved November 4, 2025.
- Pregnancy, Birth and Baby. "Nuchal translucency scan" Retrieved November 4, 2025.
- Carrying To Term. "Glossary of Diagnoses and Terminology" Retrieved November 4, 2025.
- Cleveland Clinic. "Nuchal Translucency" Retrieved November 4, 2025.
- Johns Hopkins Medicine. "First Trimester Screening, Nuchal Translucency and NIPT" Retrieved November 4, 2025.
- Illinois Department of Public Health. "Noninvasive Prenatal Testing Information for Pregnant People" Retrieved November 4, 2025.
- Radiopaedia. "Nuchal translucency" Retrieved November 4, 2025.
- Mount Sinai. "Nuchal Translucent Test" Retrieved November 4, 2025.
- The Fetal Medicine Foundation. "Nuchal translucency scan" Retrieved November 4, 2025.
- International Society of Ultrasound in Obstetrics and Gynecology (ISUOG). "Nuchal Translucency (NT)" Retrieved November 4, 2025.
- National Health Service. "Screening for Down's syndrome, Edwards' syndrome and Patau's syndrome" Retrieved November 4, 2025.
- NorthShore. "Nuchal Translucency Screening Test" Retrieved November 4, 2025.
- MedlinePlus. "Chorionic Villus Sampling (CVS)" Retrieved November 4, 2025.
- Johns Hopkins Medicine. "Amniocentesis" Retrieved November 4, 2025.
- American Heart Association. "Fetal Echocardiogram Test" Retrieved November 4, 2025.
- American College of Obstetricians and Gynecologists. "Current ACOG Guidance" Retrieved November 4, 2025.